What is giant cell arteritis (GCA)?
Giant cell arteritis (also called cranial arteritis or temporal arteritis) is an inflammatory condition affecting medium to larger arteries in people over the age of 50 years. GCA may cause headache, neck stiffness, tenderness of the temple, and/or cramping of the tongue or jaw while eating or talking. It may also cause fever, fatigue, weight loss, depression, night sweats and general feeling of illness or feeling unwell.
What causes giant cell arteritis (GCA)?
The cause of GCA is not very well understood. The inflammation from GCA is not due to infection. In GCA, it appears the body’s immune system attacks itself, in some ways similar to rheumatoid arthritis.
How is giant cell arteritis (GCA) diagnosed?
The diagnosis is first suspected by typical symptoms in an older patient. Blood tests may include complete blood count (CBC), sedimentation rate (ESR), and C-reactive protein (CRP). Biopsy of the temporal artery is necessary in most cases to confirm to diagnosis. Firmly establishing the diagnosis is critical, because treatment needs to be started quickly and continued for a long time in GCA.
The 2022 American College of Rheumatology classification criteria for the diagnosis of GCA require a total of six points based on symptoms and testing: 5 points for positive temporal artery biopsy or halo sign on ultrasound; 3 points for ESR = 50 or higher OR CRP = 10 or higher; 3 points for sudden vision loss; 2 points each for morning shoulder stiffness, jaw or tongue cramping, new temporal headache, scalp tenderness, temporal artery abnormality on exam, bilateral axillary involvement on imaging, PET scan abnormality throughout the aorta.
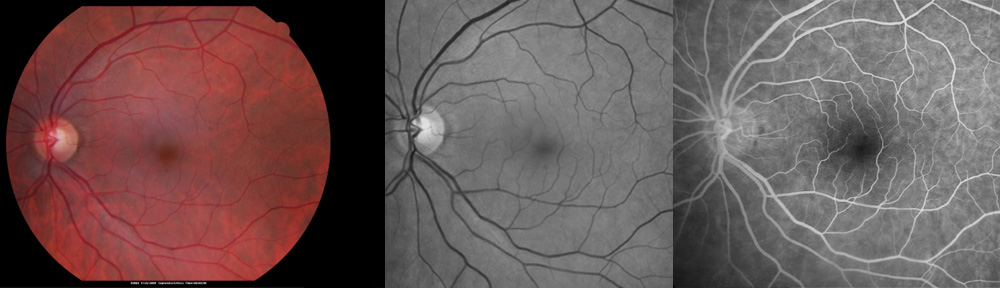
How does giant cell arteritis (GCA) affect the eyes?
Giant cell arteritis (GCA) causes loss of vision due to retinal artery occlusion or ischemic optic neuropathy. Early diagnosis is critical to begin treatment and limit the damage from blood vessel inflammation, which includes complications of brain stroke.
How is giant cell arteritis (GCA) treated?
Prompt steroid treatment is important to stop inflammation from causing further damage with loss of vision and brain stroke. Prednisone is continued at a low dose for a year or more to prevent the inflammation from returning. In an effort to avoid or manage side-effects of steroids, methotrexate is sometimes used. Tocilizumab was approved in 2017 for use in GCA. It avoids the use of steroids, but is very expensive.
Copyright © 2021-2022 Designs Unlimited of Florida. All Rights Reserved.