What is Red Light Therapy for AMD?
Red light therapy for dry-type age-related macular degeneration (AMD) is a new treatment authorized by the FDA in 2024 for the treatment of dry-type age related macular degeneration (AMD). It is delivered by the Valeda Light Delivery System to the eye. In the medical literature it is called photobiomodulation.
How does red light therapy work?
Red light therapy appears to work by increasing the energy available for retinal cells to function better. Specifically, the light (photons) is absorbed by cytochrome C in the mitochondria (the powerhouse) of the retinal cells. This increases the amount of ATP (energy) available for the retina to do its work.
Who is a good candidate for red light therapy?
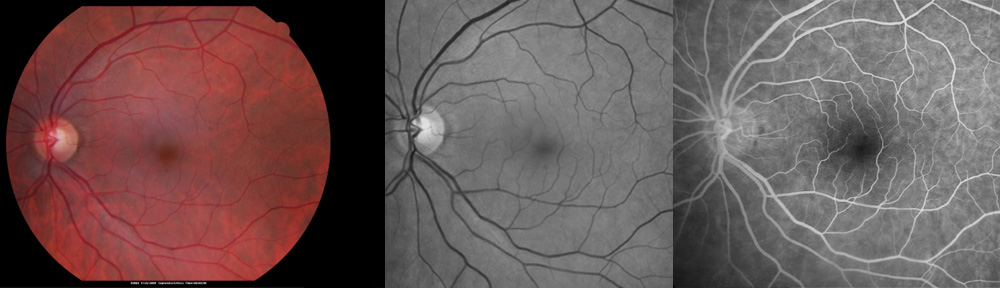
The studies included eyes with early and intermediate dry age-related macular degeneration. These are eyes with drusen deposits under the retina without profound loss of vision. Drusen deposits are hallmark of macular degeneration; they are the earliest findings to make the diagnosis of AMD.
Who is a poor candidate for red light therapy?
Eyes with advanced loss of vision from AMD are poor candidates for red light therapy. There is no evidence that red light therapy helps this group of eyes. Also, red light therapy does not help eyes with wet AMD. These are eyes that have abnormal leaking blood vessels from AMD.
How well does red light therapy work?
Red light therapy is not a cure for dry AMD, but it does appear to offer limited improvement in vision and may reduce the risk of losing vision from dry AMD. In a small study of 80 patients, red-light treated eyes were able to see almost one line better on the eye chart compared with sham treated eyes after two years of treatment. Furthermore, eyes treated with red light therapy showed a decrease in drusen and a lower incidence of geographic atrophy (advanced AMD) compared with sham treated eyes treated for two years. These are important markers that are associated with loss of vision.
What are the adverse effects of red light therapy?
Overall, the safety of red light therapy appears good for eyes with early to intermediate dry AMD based on limited data. However, it does appear that patients with any form of wet AMD in one eye may be at higher risk of developing wet AMD in the fellow eye if it is treated with red light therapy.
Should I undergo red light therapy for dry AMD?
If you have dry age-related macular degeneration, you may be helped by red light therapy to reduce the risk of loss of central vision over time. Keep in mind that we have limited evidence on safety and efficacy at this time. We have no data beyond two years regarding the need for continued treatment, as well as the safety and effectiveness of treatment. Your doctor will help you make the important decision as to whether to start red light therapy.
Copyright 2026 Designs Unlimited of Florida. All Rights Reserved.