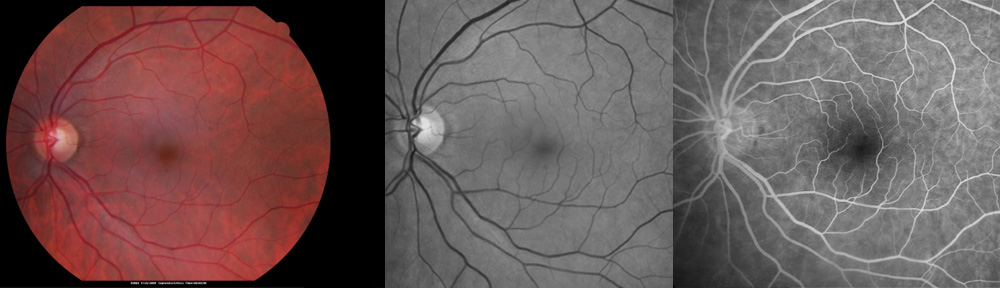
What is the difference between dry and wet age-related macular degeneration?
Age-related macular degeneration (AMD) is the most common cause of visual loss in older Americans. Doctors often talk about dry and wet types of AMD. But what is the difference? Simply put, dry AMD means there are no abnormal, leaky blood vessels. Whereas, in wet AMD there are abnormal blood vessels that grow and leak under the macula. However, this system of naming wet and dry AMD can be confusing. Therefore, newer names for the stages of AMD have been proposed.
Why is it important to distinguish between wet and dry AMD?
Dry and wet AMD cause different symptoms and are treated differently. Early and intermediate stages of AMD are often called dry AMD. These stages usually cause few symptoms, which include the need for good lighting. The treatment involves AREDS2 vitamins and a Mediterranean diet. Advanced stages of AMD are called geographic atrophy (advanced dry AMD) and neovascular AMD (wet AMD). Both types of advanced AMD are usually associated with decline in central vision, frequently affecting the ability to read, see the computer, and drive a car. Geographic atrophy (advanced dry AMD) progresses slowly with blind spots that interfere with the ability to see. Neovascular AMD (wet AMD) may advance more rapidly with distortion, blurred areas of vision, and blind spots. It is possible to have both forms of advanced AMD…geographic atrophy (advanced dry AMD) and neovascular AMD (wet AMD).
What is the treatment of advanced AMD?
The treatment of the two forms of advanced AMD is different. Furthermore, the treatment of one type of advanced AMD may aggravate the other form of AMD. However, both forms of advanced AMD benefit from the use of magnifiers and other low vision aids.
What is the treatment of geographic atrophy (advanced dry AMD)?
The Meditteranean diet is protective against advanced AMD and appears to slow the enlargement of geographic atrophy. Additionally, Geographic atrophy (GA) is currently treated with medications that inhibit the complement systems of proteins in the body that normally cause inflammation to fight infection. The two FDA-approved medications are Syfovre and Izervay. They are both given as an injection into the eye. They do not reverse the damage from GA and do not prevent GA from getting worse. They do slow down the rate of worsening of GA. There is no good evidence to show that one medication is better than the other. Long-term injections are needed over the years. And, unfortunately, both medications may cause wet AMD (neovascular AMD) to start.
What is the treatment of wet AMD (neovascular AMD)?
Wet AMD is treated with injections to stop the leaking blood vessels under the macula. These medications (Avastin, Lucentis, Eylea, Beovu, and Vabysmo) prevent further worsening of vision from wet AMD in about 90% of cases over several years. In about 40% of cases, the vision may improve. Long-term injections are usually needed over the years. There is limited evidence to suggest benefits of some medications over others. There is also some concern that the treatment of wet AMD may aggravate geographic atrophy (advanced dry AMD).
What do you do when an eye has both forms of advanced AMD?
The presence of both neovascular AMD (wet AMD) and geographic atrophy (advanced dry AMD) poses a serious problem. Both forms of advanced AMD may result in legal blindness (the loss of central vision). However, advanced AMD almost never results in complete blindness. Treatment is usually aimed at the greatest threat to vision. Specific treatment plans are made on a case by case basis. In some situations, injections are given on an alternating schedule for GA and neovascular AMD. In end-stage situations in which the chance of further loss of vision is low, all injections may be stopped. Low vision aids and assistance (family and social services) often results in high-level functioning and independence.
Copyright © 2023 Designs Unlimited of Florida. All Rights Reserved.