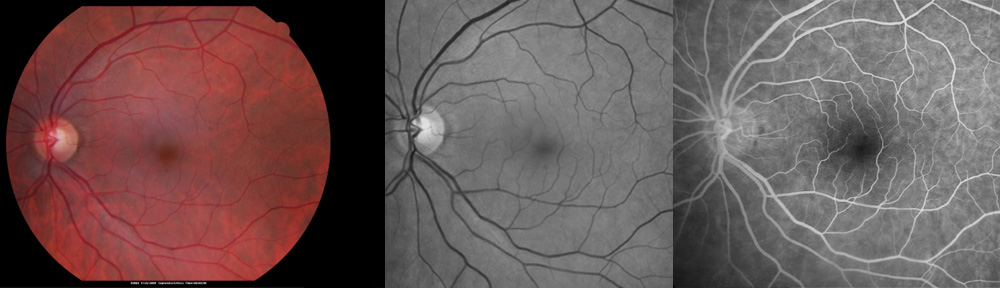
What is diabetic retinopathy?
The retina is a “tissue-paper” thin layer of nerve tissue, which lines the inside of the eye like the film in a camera. In the eye, light is focused onto the retina, which “takes the picture” and sends the image to the brain. After many years of high blood sugar, diabetes causes damage to blood vessels in the retina (diabetic retinopathy). Damaged blood vessels may leak clear fluid (edema) into the retina causing blurred vision and legal blindness. Also, new retinal blood vessels (neovascularization) may grow inside the eye abnormally. These new blood vessels tend to bleed causing floaters in the vision. In severe cases, they produce scar tissue, retinal detachment, glaucoma, and blindness or loss of the eye.
What treatment options are available?
To prevent progressive damage from diabetes, optimal diabetes management includes controlling blood sugar, blood pressure, and serum lipids (cholesterol and triglycerides), as well as weight control (diet and exercise), and avoiding tobacco. However, once diabetic damage occurs in the retinal blood vessels, laser treatment and/or medicine injections may be required. Medicine injections take effect quicker than laser, but the benefits of laser last longer than injections.
How does laser work and what are the side effects?
The laser used to treat diabetic retinopathy coagulates damaged retina and seals leaky retinal blood vessels. Laser treatment may be given in the office or the operating room and is usually well tolerated with minimal discomfort. Side effects may include difficulty with night vision, side vision, and, rarely, central blind spots. Many of the same side effects appear from diabetes over time as blood vessel blockage occurs from high blood sugar levels. Indeed, although there were concerns about loss of peripheral vision following laser for advanced (proliferative) diabetic retinopathy, we now know that loss of peripheral vision occurs in this setting even without laser treatment.
How do injections work and what are their side effects?
Injections of medicines are divided into steroid medicines and non-steroid (anti-VEGF) medications. With any injection, there is a low risk of serious infection that may blind the eye. Non-steroid (anti-VEGF) medications work by blocking chemical messages between retinal cells that cause leakage and bleeding in diabetes. Anti-VEGF medications include Avastin, Lucentis, Eylea, and Vabysmo. These medications take effect fairly quickly and are very effective, but the effect does not last very long (unlike laser). Anti-VEGF injections must be given every 4-6 weeks at first. Over months to years, fewer injections are usually needed. There appears to be an increased risk of death from stroke and heart attack among patients who undergo repeated antiVEGF injections for up to 2 years. The risk is about 17% (range: 2% to 33%) higher in diabetics undergoing injections than other diabetic patients not undergoing injections.
Steroid medicines are effective, but are generally considered a second-choice medication because of side effects. They are given by repeated injection. Side effects include a very high chance of cataract over a period of months to years. Steroids may cause the pressure in the eye to rise and this may result in glaucoma, which requires eye drops and may require surgery.
When to use injections and when to use laser?
The two main reasons to undergo treatment for diabetic retinopathy are 1.) swelling of the retina (macular edema) and 2.) the growth of abnormal new blood vessels (neovascularization) that threaten to bleed into the eye. Macular edema occurs when diabetes causes a breakdown of the normal water-tight barrier in the walls of blood vessels in the retina. If edema is located in the center of the macula, injections have been shown to be superior to laser. However, supplemental laser treatment may help to seal leaks after the injections begin to take effect. If macular edema is not located in the center of the retina, laser alone may protect against loss of vision. Injections may be added later if edema extends into the center of the retina at a future date.
Neovascularization (NV) is the new growth of abnormal blood vessels on the surface of the retina. The growth of these blood vessels indicates an advance degree of damage to the retina from diabetes. This stage of diabetes damage is called proliferative diabetic retinopathy. NV causes loss of vision from bleeding (hemorrhage), scarring, and retinal detachment. NV may be treated with laser and/or anti-VEGF injections. If center-involved macular edema is present along with NV, anti-VEGF injections are usually preferred at the start of treatment. However, anti-VEGF injections may be used alone in the treatment of NV in the absence of macular edema, as well. But the injections must be given monthly at first, and the eye must be rigorously monitored. If there is a gap in treatment, the result may be disastrous. If there is a gap in treatment, the risk of vision loss is less if the patient has had laser as opposed to injections alone.
Laser has been used successfully for long-term control of NV since the 1970’s. Laser is performed in the office or the operating room and is well-tolerated. Usually, one to three treatments offer long-term control of NV. Laser is currently considered a standard treatment for NV in the absence of center-involved macular edema. However, anti-VEGF injections remain an option, as well. The advantages and disadvantages of each form of treatment must be weighted in a given case. In some instances, a combination of injections and laser may be preferred. Unfortunately, despite these treatments surgery in the operating room may be needed. Although vision is usually preserved with treatment, diabetes remains the leading cause of blindness in the United States. The best results of treatment are seen in patients who have regular eye exams and manage their blood sugars well.
By Scott E. Pautler, MD
Copyright © 2019-2025 Designs Unlimited of Florida. All Rights Reserved.