What is myopic macular degeneration?
Myopic macular degeneration (MMD) is a degeneration of the center of the retina seen in some people who are myopic (near-sighted). MMD is not the same as age-related macular degeneration. The macula is the area of the retina in the back of the eye that is responsible for seeing details in the central vision. The retina is a thin layer of delicate nerve tissue that lines the inside wall of the eye like the film in a camera. In the eye, light is focused onto the retina, which “takes the picture” and sends the image to the brain. Although macular degeneration affects the central vision, it does not affect peripheral vision— the ability to see objects off to the side when looking straight ahead. This means that macular degeneration alone does not result in total blindness.
What causes myopic macular degeneration?
Changes in the shape of the near-sighted eye cause myopic macular degeneration. The normal shape of the eye is round like a ball. As an eye becomes myopic, the eye elongates and looks more like the shape of an egg. The elongation of the eye means that the retina becomes stretched and thin. This causes macular degeneration in some eyes over time. The higher the amount near-sightedness (the thicker your glasses), the greater the chances of myopic macular degeneration. Two forms of MMD are “dry” and “wet”. However, the wet type may become “dry” and the dry type may become “wet” over time:
- Dry macular degeneration is the most common type and involves the disintegration of the light-sensitive tissues in the macula. Loss of vision is usually gradual in dry macular degeneration.
- Wet macular degeneration occurs in a small group of eyes with MMD. It occurs when abnormal blood vessels grow under the macula and cause fluid leakage, bleeding, and scarring of the macula. Vision loss may be rapid and severe. An important, but under-recognized form of wet MMD is dome-shaped maculopathy.
What are the symptoms of myopic macular degeneration?
Macular degeneration may cause no symptoms in its early stages. Over time, symptoms may include the need for more light while reading and blurring of central vision, often with distortion or a blind spot. Although macular degeneration is usually present in both eyes, it may cause visual symptoms in only one eye. Rarely, severe loss of vision occurs in both eyes, and render a person legally blind. However, total blindness is extremely rare in myopic macular degeneration.
How is myopic macular degeneration diagnosed?
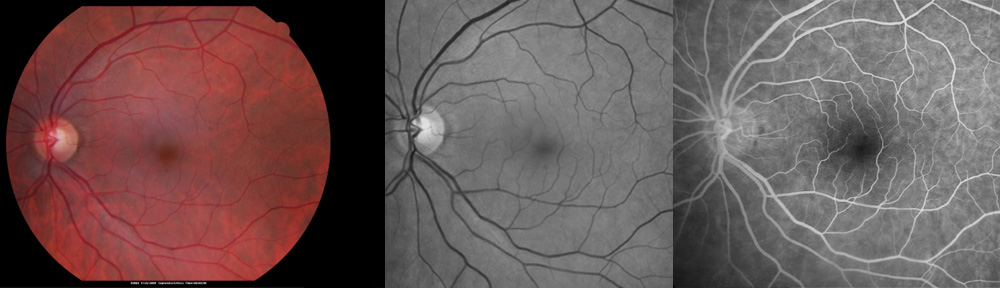
A dilated eye examination can detect myopic macular degeneration before visual loss occurs. The hallmark of myopic macular degeneration is a thinning of the macula due to stretching of the retina and the underlying blood vessel layer that gives nutrition to the retina. After the diagnosis is made, a fluorescein angiogram is often helpful. In this procedure the ophthalmologist injects an organic dye into the vein of the arm. Photographs of the retina are taken to reveal the presence and location of the leaking blood vessels marked by the organic dye.
How is dry myopic macular degeneration treated?
No specific treatment is required for eyes with MMD and no symptoms. However, it may be helpful to avoid eye rubbing. If the eyes feel tired at the end of the day, warm compresses are safer than rubbing the eyes. A Bruder mask may be purchased at the drug store or online. It may be heated in the microwave for 10 seconds and placed on the eyes after testing the temperature. It provides warm moist heat that soothes the eyes.
How is wet myopic macular degeneration treated?
Medication injections (Avastin or Lucentis) performed in the office often help preserve vision in wet MMD. Treatment rarely returns vision to normal, but may limit the amount of vision loss from blood vessel growth and leakage. Frequent office visits and photographs are needed to monitor for activity and determine the need for treatment. The Amsler grid test is used at home to help monitor the vision. If the grid test shows new or progressive distortion in the vision, notify the eye doctor within a few days.
Please note: As an Amazon Associate I may earn from qualifying purchases. You pay no additional fees by accessing the link provided. These funds help defray the costs of maintaining this website. Thank you for your support.
Copyright © 2019-2023 Designs Unlimited of Florida. All Rights Reserved.